Background and rationale: modular structure
This curriculum describes Core Surgical Training in the UK. Arrangements in the Republic of Ireland differ, although some aspects are the same (e.g. the syllabus content for the MRCS examination). The overarching content of the Intercollegiate Surgical Curriculum Programme (ISCP) forms the basis for this curriculum but it has been updated and modified in parts to reflect aspects specific to Core Surgical Training.
The syllabus element of this curriculum, together with a brief explanation of its modular nature, has been inserted into each specialty curriculum.
BACKGROUND and RATIONALE
Core surgical training is diverse. Uncoupled from specialty training for the majority of trainees, the neurosurgical curriculum describes a run-through programme for all ST1 entrants and Cardiothoracic Surgery, Trauma and Orthopaedic Surgery (T&O) and Oral and Maxillofacial Surgery (OMFS) curricula are divided with both run-through and uncoupled programmes currently in operation. In addition, Academic Clinical Fellowships grant run-through status to successful applicants. While some Core Surgical Training programmes provide pre-agreed 2 year rotations themed to one of ten specialties, others are generic. In recognition of the time spent in dental surgery by its trainees, OMFS training omits the CT2 year. The required final competencies of successful trainees are also diverse with each specialty having its own expectation of a new ST3 trainee represented in distinct recruitment person specifications. Despite this diversity, there remains a commitment to retain within core surgical training a generic training in that which is common to all surgical practice.
This 2017 update to the curriculum for core surgical training aims to serve multiple diverse training needs and satisfy multiple distinct stakeholders in a single document. Contributing to its content and design has been the uncoupling of core surgical training from specialty training for all the surgical specialties bar neurosurgery, crystallisation of single centre national recruitment, the introduction of the specialty of vascular surgery, three minor syllabus revisions in 2010, 2013 and 2015, continued national devolution and for England, the creation of Health Education England and its Local Education and Training Boards and geographies.
Both active trainers and current trainees have been involved in the preparation of this curriculum, through their representatives at the Core Surgical Training Committee and all ten Specialty Advisory Committees (SACs) of the Joint Committee on Surgical Training (JCST). The patient voice has been sought through the lay members of JCST. The Intercollegiate Committee for Basic Surgical Examinations is responsible for delivery of the MRCS exam, a mandatory component of the scheme for assessment of this curriculum, which will need to blueprint against it. Each SAC has produced a set of quality indicators for core training posts in their specialty. Each national specialty recruitment team, within which the SACs are heavily represented, have their own ST3 person specifications; these documents and this curriculum align with each other. Each specialty curriculum currently includes a specification for early years training and it is intended that this 2017 revision of the Core Surgical Training (CST) curriculum will unify these surgical curricula elements.
Curriculum structure
In order to satisfy the many diverse requirements and stakeholders laid out above in a single document, this curriculum has adopted the flexibility of a truly modular structure. At its heart are the educational principles, assessment tools and supervisory framework of the current intercollegiate surgical curriculum, which are here applied to the specific requirements of core surgical training. In addition to the professional behaviour and leadership skills module common to all ISCP curricula, there are three types of module:
Common content
Those items of knowledge and clinical and technical skills which represent the generic competence required of all future surgeons are represented in a module to be undertaken by all CT1 and ST1 surgical trainees. The MRCS examination aligns to this module which serves to define the CT1 competencies required by the OMFS ST3 person specification. It is here that those competencies transferable to other training programmes are to be found.
Core specialty
As they rotate from specialty to specialty in years 1 and 2, trainees will take on the relevant core specialty modules, which will specify the knowledge and skills that all surgical trainees in such a placement should acquire, regardless of their surgical specialty of choice. These modules align with the quality indicators suggested by the SACs for core training posts in their specialties. Most trainees will wish to complete at least three of these modules, one of which will be in the same specialty as their ST3 preparation module.
ST3 preparation
By the start of their CT2 year, trainees in uncoupled programmes should have made a choice regarding the specialty in which they wish the rest of their career to develop. Run-through trainees will already be bound to a specialty. Starting in their second year, trainees will work towards completion of the ST3 preparation module in their chosen specialty. These modules align with the entry expectations of the higher surgical training programmes and with the essential criteria of the person specifications of the ST3 national recruitment panels.
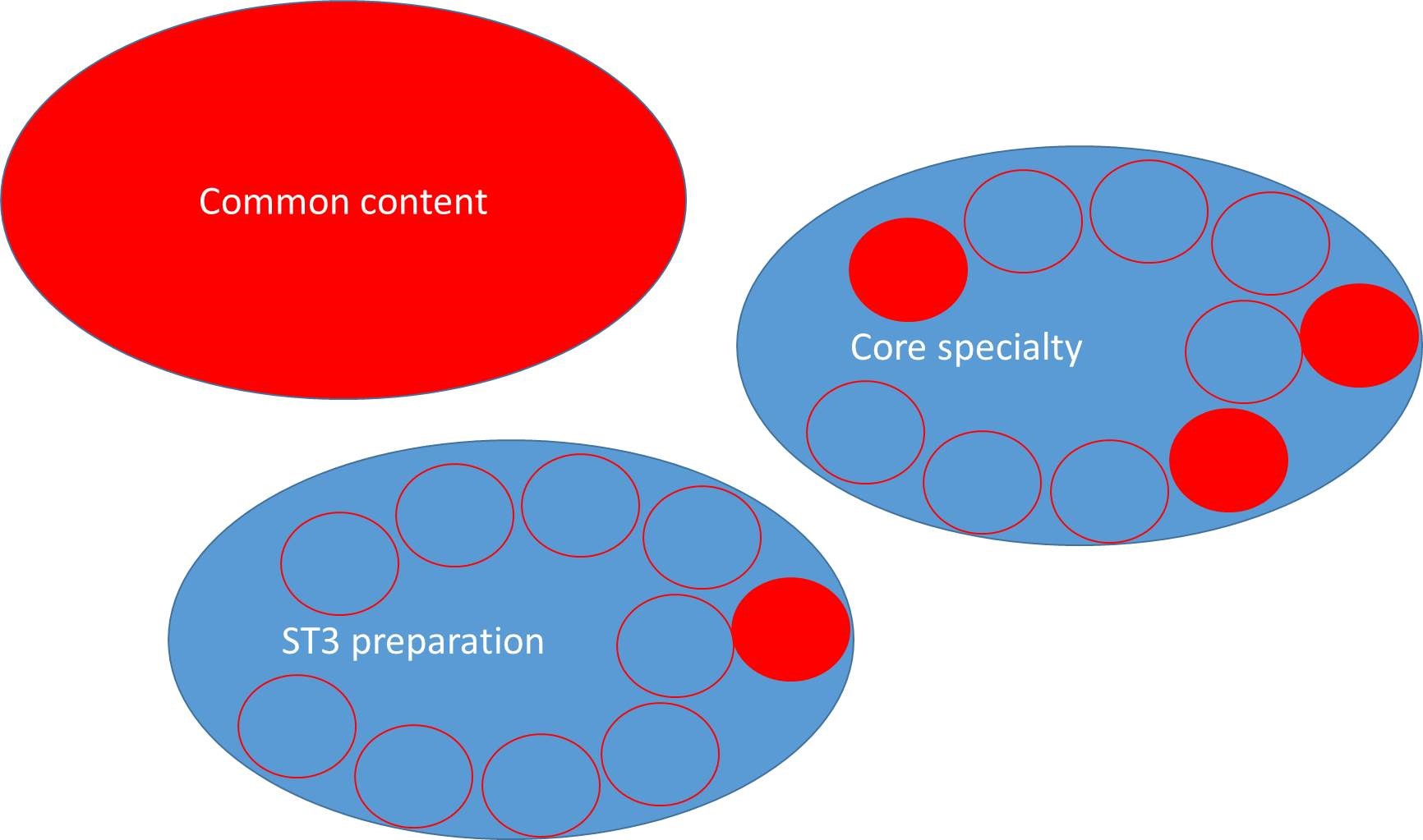
The minimum requirements for this curriculum are completion of the common content module, the core specialty module for each specialty through which the trainees rotate (which may be as few as one) and one ST3 preparation module (which may be in any specialty of the trainee's choice).